PEMFs Reduce Progression of Arteriosclerosis
Table of Contents
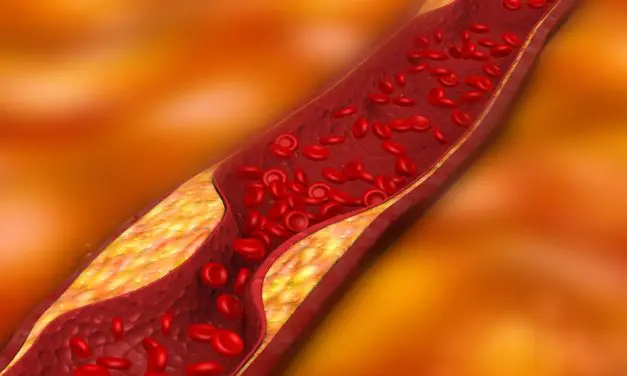
Vascular disease within the heart and throughout the body is one of the top causes of death and disability. Additionally, most vascular disease is associated with blockages of blood vessels, called arteriosclerosis or atherosclerosis. Atherosclerosis is a leading cause of vascular disease worldwide. Its major clinical manifestations include ischemic heart disease (IHD), stroke, and peripheral arterial disease (PAD). Moreover, atherosclerosis is a progressive disorder, developing with age. The incidence of PAD is 1% at age 40 to 49 years and 15% at age ≥70 years. The incidence of ischemic stroke in the United States for 2010 was 143 per 100,000 person-years. The IHD risk of death is 200/100,000/year. Many factors lead to arteriosclerotic vascular disease. Controlling cholesterol is one of the most common strategies, but it is not a reliable method of reducing the progression of arteriosclerosis. So, can PEMFs be used for this purpose?
Bypasses and stents are commonly used to provide circulation around a blood vessel blocked (stenosis) by atherosclerosis. These bypasses have the same risk of becoming blocked as the rest of the vascular system. This is called restenosis. Nonetheless, restenosis often happens very rapidly compared to the gradual progression of stenosis in the general vascular system.
PEMF STUDY ON VASCULAR DISEASE
I discovered a study from 2003 where a relatively low intensity of 700 micro Tesla (7 Gauss) 50 Hz magnetic field was meticulously studied in mice, which had undergone a vascular bypass operation. Firstly, in mice, thickening of the inside lining of the blood vessel (intima) is seen as early as one week after bypass. This thickening usually increases an average of 10-fold after just four weeks and 15-fold after eight weeks. The mice received either active or sham PEMF treatments for two hours a day, five days a week for one, two, or three weeks. The mice were positioned about 12 cm away from the magnetic field coil.
Mice exposed to the PEMF for one week had significantly less intimal thickening compared to the sham field. However, intriguingly, those mice exposed for two or three weeks showed no differences, although, at three weeks, the sham mice had a higher level of thickening.
This study evidently shows that even a very low intensity PEMF of 700 micro Tesla has a modest amount of impact in slowing the initial progression of atherosclerosis. Nevertheless, a major drawback of the study is that, while 700 micro Tesla was used, the actual magnetic field delivered to the mouse would be less than one micro Tesla. Consequently, since the process of progression is likely more aggressive than the benefit received from the PEMF beyond one week, it may be reasonably assumed that higher intensity PEMFs would provide more substantial benefit.
Extending research results from mice to humans is always challenging, but changes happen in mice much faster than in humans, so it can also be reasonably assumed that long-term use of higher intensity PEMFs in humans would be undoubtedly effective in reducing the progression of the atherosclerosis that leads to ischemic heart disease, stroke, and PAD. Additionally, other research, such as that by Jerabek, unquestionably shows that PEMFs can significantly improve vascular disease in humans.
References
- Progression of arteriovenous bypass restenosis in mice exposed to a 50 Hz magnetic field. Henderson B, Tagwerker A, Mayrl C, et al. Cell Stress Chaperones. 2003 Winter;8(4):373-80.
- Jerabek J, Pawluk W. Magnetic Therapy in Eastern Europe: A Review of 30 Years of Research. Chicago, IL: Advanced Magnetic Research of the Delaware Valley, 1996.