Scleroderma
Table of Contents
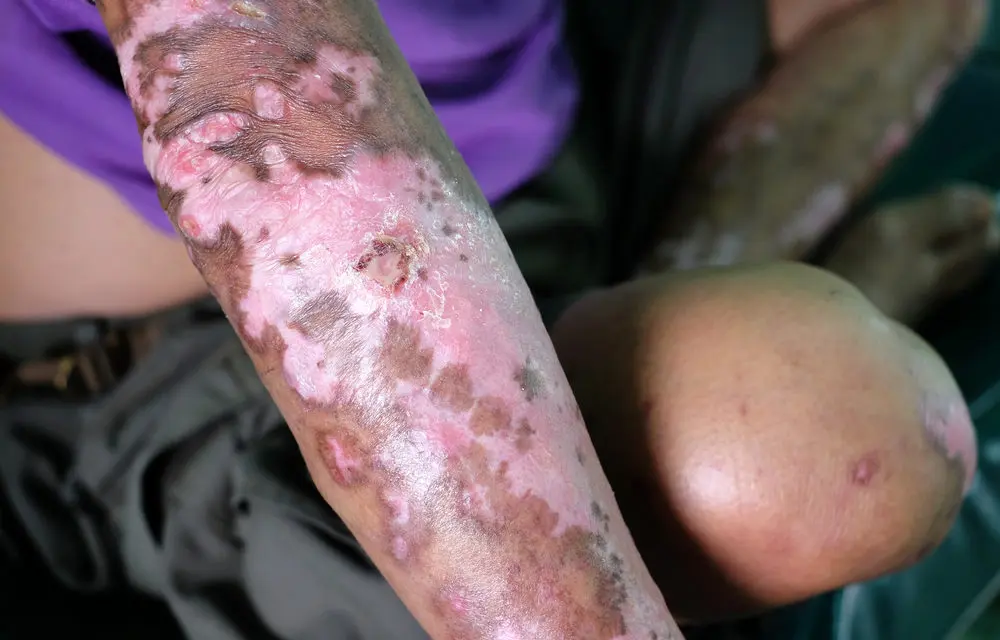
WHAT IS SCLERODERMA OR PROGRESSIVE SYSTEMIC SCLEROSIS (PSS)?
Scleroderma or progressive systemic sclerosis (PSS) is a very complex condition, with a major autoimmune component. Food allergies need to be ruled out as a potential cause. Pulsed electromagnetic fields (PEMFs) may be effective for controlling certain aspects of scleroderma. However, it would not be expected to cure or turn off the condition. Basically, PEMFs would be very helpful to control some of the complications and side effects of the scleroderma. It may actually slow down its progression. There is no reason that it could not be used alongside any other therapies, including disease modifying regimens. I was able to find two studies that evaluated its use. I have no testimonial experience treating this condition.
PEMF STUDY IN PATIENTS WITH SCLERODERMA
The first study comes from my book. 20 scleroderma patients with Raynaud’s syndrome were treated with a PEMF applied to the spine at C4-Th7 and Th10-L2 vertebrae. They found that 95% had improvement in excess of palmar sweating, cold sensitivity, reflexes and ulnar nerve conduction. Velocities increased by 5-7m/s.
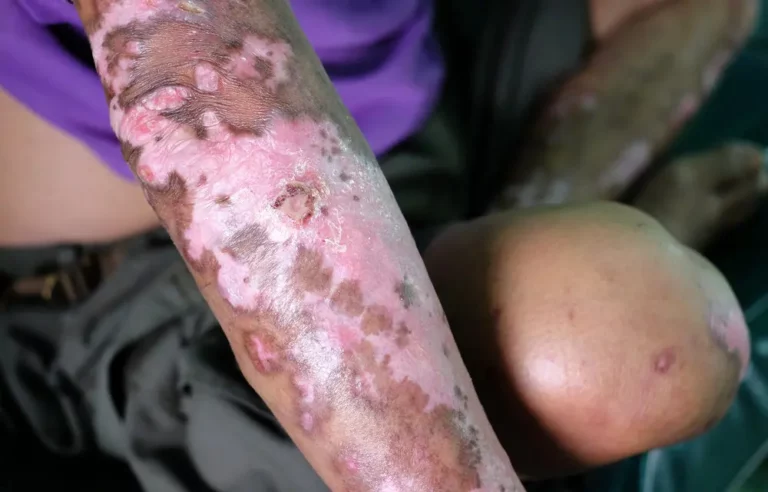
The second controlled clinical trial looked at treatment with a different PEMF in combination with other conventional and alternative therapies, which included physical therapy, supplements, and massage. This study had 80 patients, 52 of whom had local thickening/induration and 28 head multiple areas involved. The study had a basic group and a comparison group, with 40 in each, and a third control group of healthy people. The therapy group had the usual therapies plus PEMFs, whereas the control group only had the usual therapies.
Treatments were applied every other day for a course of 12 procedures. They were evaluated using clinical and immunological testing. The treatment group had full recovery in 16 of 40 individuals, with significant improvement in another 22 (95% showing at least some improvement). The control group had full recovery in only 10 and significant improvement in 19 (73% showing at least some improvement). There was a highly statistically significant improvement in immune indices compared to the control group, including immunoglobulins, blast transforming activity of lymphocytes and complement. They concluded that PEMFs facilitate clinical as well as immunological improvements in scleroderma/PSS.
While these studies indicate benefit in scleroderma patients with even a limited course of use, it would be expected that continuing benefit would be seen with continued use over the long-term. It may be necessary to continue traditional disease modifying agents (DMARD treatments) at the beginning, depending on the severity of the scleroderma, and then gradually taper them off with continued PEMF use and monitoring of clinical parameters. Adding oral type I collagen supplementation to the treatment protocol may also add to the benefit of PEMF’s to improve the thickening of the tissues, since PEMFs, have been found to improve scars caused by aggressive collagen deposition.