Urinary Stress Incontinence Improved By High Intensity PEMF Therapy
Table of Contents
WHAT IS STRESS INCONTINENCE?
Stress incontinence, primarily urinary, is a very common problem in women of childbearing age and older. Treatment is either nonsurgical or surgical. Nonsurgical treatment includes biofeedback, vaginal cones, and electrostimulation, with success rates ranging from 9-63%, side effects and embarrassment from probe insertion into the vagina. The gold standard surgical intervention is a mid-urethral mesh sling which has a success rate of 56-98% at one year. Unfortunately, about 6% require further surgery, 15% do not respond and 8% are surgical failures at five years. At nine years about 15% of women need repeat surgery. There have been about 75,000 lawsuits against mesh manufacturers due to false and misleading information about safety and effectiveness.
HOW CAN PULSED MAGNETIC FIELDS HELP WITH STRESS INCONTINENCE?
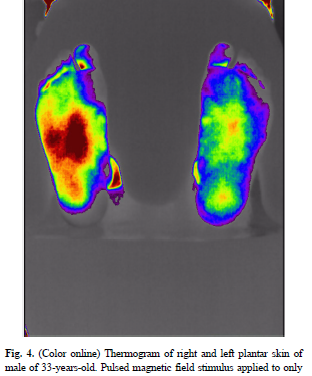
High-intensity pulsed magnetic field (HIPMF) stimulation of the pelvis has been available as a non-surgical option since 1998. It has the advantage of not requiring disrobing, insertion of electrical probes or continuous exercises. HIPMF given to women sitting on a PEMF coil penetrates deep into the pelvic floor, providing nerve and muscle stimulation. The pelvic muscle contractions are not uncomfortable and lead to strengthening of the pelvic floor muscles, thus reducing the symptoms of incontinence. While these contractions are similar to Kegel exercises they are much more complete and more intense.
A STUDY OF PEMFS AND STRESS INCONTINENCE
A recent study reported on the treatment of 120 women, half of whom received either active or sham PEMF stimulation. The sham stimulation was actually a much weaker active PEMF signal which could still be felt. Treatment was for 20 minutes twice a week for 16 sessions. After two months women who were not responding or not satisfied could opt for 16 additional sessions. Outcome measures were international consultation on incontinence questionnaire (ICIQ-UI SF) and various physical measures of continence.
At two months, 75% receiving active stimulation were treatment responders versus 22% receiving sham treatment. A little more than ½ of the women received an extra 16 sessions of stimulation, that is, up to four months of treatment. When they were assessed at 14 months after the start of treatment, those who received 32 sessions of active treatment had a 75% response rate, followed by those who had only 16 sessions [68 – 72%]. At the end only 19 of 60 women did not get any active stimulation, but, still had a final response rate of 21%.
This study shows that high intensity PEMF training of pelvic muscles for stress incontinence has a 68 – 72% success rate at about a year following treatment with 16 treatment sessions, improving slightly to 75% in women with 32 treatment sessions. Results appear to show that 16 sessions of stimulation give impressive results at the end of treatment but, as might be expected, some women lose this benefit after about a year. This would indicate that “tuneups” may be necessary periodically to maintain benefit.
The value of PEMF pelvic muscle training for stress incontinence is that it is safe, nonintrusive and convenient. The downside is the need to go to a professional for treatment, which may or may not be covered by insurance. A home-based PEMF system with a sufficient intensity to cause pelvic muscle contractions could potentially be effective as well.